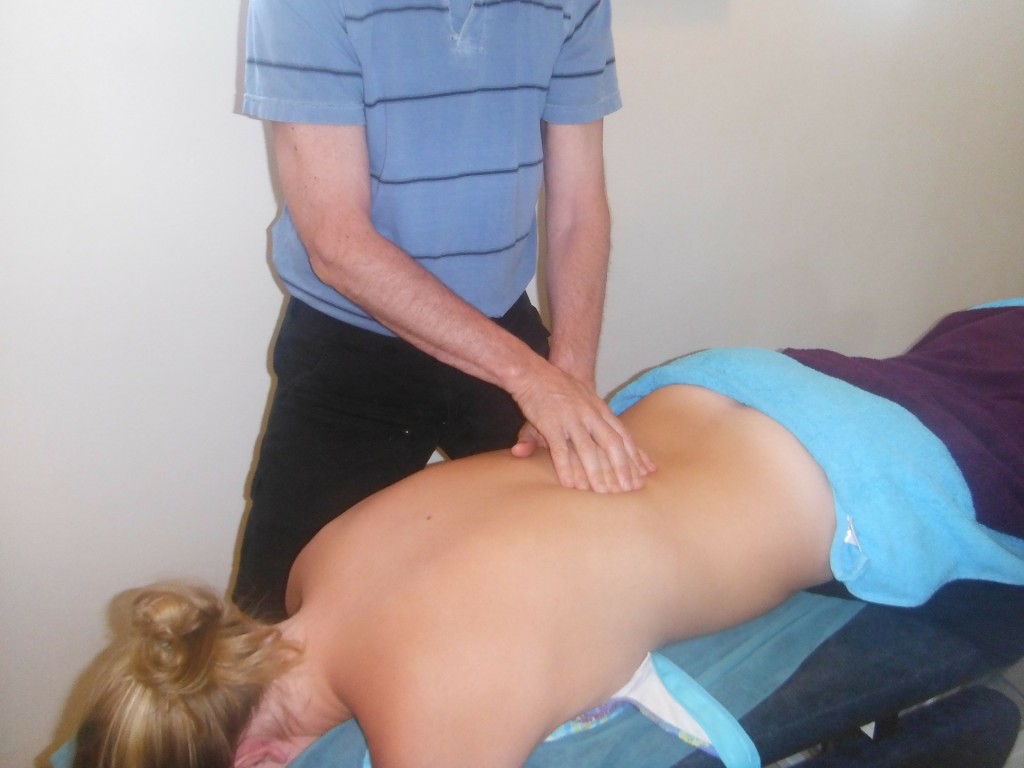
Over the many years at our active Vancouver clinic our daily patients always comprise of a significant portion of people with neck and low back spinal pain. The statistics for the incidence of low back pain may vary depending on where you find them, but a significant percentage of the patients seen by doctors and physiotherapists today have low back pain. For instance, in 2012 WorksafeBC put out a report and it showed that from 1980 to 2012 the proportion of work related back strain injuries reported to all injuries has ranged between 22% to 26%. Although two thirds of those affected were men a decade ago, the gap has narrowed in recent years between the genders. All ages are affected by low back strain injuries, but most commonly peaked between the ages of 35 and 44.
Most low back injuries will recover and heal in a short period of time. They may be muscle and ligament sprains and strains, and if protected and rested during the acute phase then gradually returned to activity, the back pain usually resolves. In the clinic I will see the early very painful low back injuries, and more frequently the ones that don’t resolve and become chronic. The chronic cases of low back pain are much more complicated in nature and require a very active approach between the patient and physiotherapist/doctor in order to be successful.
4 common questions patients will ask me in the initial assessment are:
1. What Is Injured and Is It Serious? What Is Causing the Pain?
To find out precisely what the problem may be, it is important that the patient gives good verbal history of what activity or movement was done when the pain appeared, the location and type of pain is felt, how intense or easily irritated is the injury, what movements aggravate and ease the pain and so forth. Doing a physical examination can give us clues to what may be causing the pain, but often times it is very difficult to pinpoint the exact structure in the body that is hurt. More importantly, knowing the patterning and characteristics of the pain, and a thorough physical examination is invaluable to treating the injury and pain successfully. Muscles and ligament injury, vertebral joints stiffness and injury, disc hernia and injury, sacroiliac joint dysfunction and sprain (pelvic joints) are all common in low back pain.
2. Should I Go See My Doctor and Get an Xray or MRI?
I always recommend that the patient discuss this part with his/ her family doctor together to further determine the need for an xray or MRI. I will often send a note to the doctor to give my physical findings to help the doctor further determine this need for an xray or MRI.
In the many cases I have seen, an xray or MRI is not needed simply because:
i) the injury is healing and further radiation and wasting of time/ resources is not necessary,
ii) there is sufficient findings from the verbal history and physical findings to properly treat the area,
iii) often times an xray/ MRI may show some findings but is very difficult to correlate these findings specifically to the actual pain and symptoms felt,
iv) and there are no obvious red flags that would prompt for further investigations.
Red flags may include nerve pain in the legs accompanied by remarked weakness, bowel and bladder symptoms, pain and numbness in bottom of the pelvis, unrelenting pain especially during the nite, etc.
3. What Can Physiotherapy Do For It? What Can I Do and Not Do and How Long Will It Take to Recover? When Can I Return to Work or Play Tennis (For Example)?
From the assessment the physiotherapist determines what the injury may be and can use an array of methods to start resolving the pain and promote recovery.
i) Ultrasound, electrotherapy and laser therapy can be used for pain and/or inflammation alleviation, and promote recovery.
ii) Manual therapy is when the physiotherapist mobilizes or manipulates the joints of the spine to promote proper spinal movement and alleviate pain.
iii) Short duration and more prolonged traction of the spine (by the therapist, or traction machine) can help with pain and recovery of the spine and nerve pain.
iv) Acupuncture and IMS (intramuscular stimulation) needling can be used for inflammation, release and normalization of muscle tone, nerve pain and sensitivity.
v) Exercise prescription is key for strengthening and long term recovery in almost all cases. Most systematic studies for treatment show that a multimodal treatment approach (combination of treatment types and exercise) is the most successful approach.
4. Why Know More?
Perhaps the most important part of managing an injury is education. This means learning about the probable causes and what can be done to manage it. For instance, central low back pain due to muscle tightness can resolve very quickly over a couple weeks and the person can return to tennis pretty quickly. In contrast, low back pain from a disc injury that is causing nerve pain down one leg may take a several months to alleviate and strengthen to prevent further injury, especially for tennis where there is a lot of twisting and bending of the trunk during play.
Finally, an important inherent characteristic to success is a positive outlook and willingness to participate in the process of recovery!
Carman Wong
Physiotherapist (BCScBiol, BCScPT, FCAMPT, CG*IMS)
Extensive experience in treating neck, shoulder, lower back, knee and motor vehicle accident related pain.